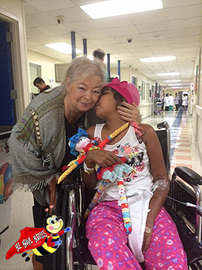One week post-election, I found myself bound for Mexico City, ready to teach and learn alongside my adventure colleague, Maria Busqueta. Marifer, (as I call her) hosted me in her home town, where she is a child life specialist, psychologist and educator. It was a whirlwind couple of days, as we visited the General de la Raza Hospital, learned about the Ayudarme a Sonreir ante el Cancer Foundation, The Vuela Foundation, taught a class on play techniques for adolescents, and attended a two-day conference on palliative care. Phew!
My first impressions of Mexico City and Marifer’s neighborhood: Unexpectedly cold and wet. Lovely hills rising up from the urban center. Cypress trees in plenty and Bougainvillea in bright, fuscea explosions amongst the trees and spilling down high stone retaining walls. Hilly, winding roads with speed bumps everywhere instead of stop signs. Heavy and erratic traffic. Cold mornings and nights. Marifer’s house has many levels to it, all encased in gingerbread auburn ceramic tiles. Like my home, the kitchen and living room are on the upper level, with bedrooms below. Marifer’s jaunty beagle, Duncan, lords over the front yard and threatens escape with each coming and going of a human being through the iron gate. Marifer’s mother cooks for us several times a day, filling me with homestyle Mexican fare. It is mere moments before I feel like family.
We are up bright and early my first full day there, ready to pay a visit to the Hospital Raza. Lisette Garcia Urenda, the founder of the Ayudarme a Sonreir ante el Cancer Foundation (which translates as “We help you smile after cancer”), is hosting us, and we meet her outside of the largest and oldest public hospital in all of Mexico. The sidewalks surrounding the building team with merchants hawking their wares, everything from pork roasting in a cauldron to magazines and fruit. We weave past the stalls and in through the back emergency entrance to the hospital. As we enter the foyer, several pediatric cancer patients and their families are exiting the hospital, bundled up for discharge and eager to be home. But they stop to hug, kiss and chat with Lisette. They shake our hands and offer “mucho gusto” as Lisette introduces us.
It is clear that the children and their caregivers adore Lisette. And it is easy to see why – she is all brightness, high energy and love. One teenage boy jokes for me to take him back to the United States with him. The younger children glance at us shyly.

There are three events planned for the day, two presentations to patients and a therapeutic art activity to be conducted on the inpatient ward. The foundation grants wishes for pediatric cancer patients, and families have gathered to witness Lisette’s presentation of a wish to a young girl. They sit in tiny, child-sized plastic chairs around the parameter of an open roofed waiting area. The children sport face masks, bald heads, hats, and winter coats with good reason. It is cold.
The child is brought to the center of the room, and Lisette introduces her to everyone. I am regretting in the moment that I don’t understood more Spanish, but it seems that she is telling them how well the girl is doing post bone marrow transplant. With great flourish, Lisette hands the girl a large present. The child opens it with excitement and beams at its contents, an “alien” doll that is apparently quite the rage. It’s hard not to note what a child with cancer might have in common with the toy. Both are bald; both might need to be isolated because of threatening germs in a hostile environment; both may need to be fed through a tube in the stomach. And, any child who has such a diagnosis may often feel like a misunderstood species hovering over the more typical lives of healthy peers.
The child hugs Lisette. The onlookers clap, and I wonder if they are envious of her. Lisette explains to me that most of them will have a wish granted at some point, so that no child feels left out. Later, the child’s mother is crying in the hallway, sharing bad news with her social worker. Her daughter has relapsed. The bone marrow transplant didn’t take.
Lisette says that many of these children die, and that in order to do her work, she must get lots of therapy and continually study and obtain higher degrees. This is why she is a current student of Marifer’s. She does the work because when her father-in-law died, he told her that she must work for the forgotten children. She says that many of these children don’t have electricity in their homes.
The next planned event is the presentation of a natural hair wig made from five individual donations of hair. The recipient is a six-year-old girl. She is very shy and quiet. We are in a hall outside of the infusion clinic. The floors are buckled and seams of cement overflow the protruding tile. I wonder if this is from an earthquake. Nurses wear white and institutional green uniforms, donning plastic nursing caps in the same colors. I feel like I have stepped back into the 1950’s, except for the fact that they are all taking photos on their cell phones as Lisette presents the wig to the child.
Lisette speaks with the girl for quite some time. She reassures her that she needn’t speak if she doesn’t wish to, that they can communicate with their eyes. Lisette tells the child about the beauty of her heart, that the wig is just an accessory, that her beauty is not dependent on whether or not she has hair.
You must say to yourself every day in the mirror: “I am beautiful!”
The child tries on the wig and looks in a mirror provided by Lisette. Everyone poses for photos with her. In the end, her mother repacks the wig carefully in the box, and they are on their way.
Lisette leads us through a chaotic and crowded hallway to a packed elevator that carries us to the inpatient pediatric oncology unit. In the hallway between two separate wings (one designated for solid tumors, the other for liquid), is a small but well equipped playroom. Siblings and patients mingle at child-sized tables. There are floor to ceiling shelves laden with cause and effect toys, a toy hospital, dollhouse, action figures (“for boys” says the playroom coordinator), blocks, puzzles, games and art materials. There is a large dollhouse in a corner, a kitchen play set, and several large bookcases overflowing with books. Lisette’s foundation supplies the DVD lending library. One child sits with an adult working on a puzzle. Another plays with the dollhouse. A mothers group meets in the waiting room next door. The only thing I feel is missing is a medical play corner and sensory play materials. A flatscreen tv plays a Disney movie overhead.
Lisette has plans for an expressive arts activity. She brings us to the liquid tumor wing, into a room with six beds. Five children between the ages of two and fourteen seem excited to see Lissette and very open to our visit. The six-year-old boy is talkative and funny. After some quipping back and forth, Lisette hands out crayons and art paper to the children with a body outline on it. But before she can begin to explain the instructions, the two year-old’s mother leaves the room, and the toddler begins to cry loudly and inconsolably . She sits in her cage-like crib, crying desperately, reaching both arms up as if asking her absent mother to pick her up. Either that, or she is imploring the Gods to bring her mother back!
Lisette approaches with kind words, but the toddler is having none of it. She screams louder. Lisette offers her crayons and a “Frozen” coloring book. The child cries “No!” and turns away. Lisette is unperturbed. Using the surroundings, she jumps quickly into a bit of improv. The room has been newly decorated with a brightly colored mural on all four walls, ceiling to floor. It is a nature and farm scene. Near the girl’s bed, close to the floor, a mother duck swims with her three ducklings on a bright blue pond. Lisette launches into a conversation with the ducklings, turning her back on the toddler, lessening the child’s stranger anxiety by ceasing direct eye contact. She engages everyone in the room in asking the names of the ducks. She suggests the proffered names, and the little girl shakes her head in protest at each one. But she has stopped wailing and is watching Lissette intently. Lisette blocks the child’s view of the mother duck and tells a tale of the ducklings searching for their mother. She reassures the girl that her mommy will always return. We all sing the song “Five Little Ducks”. Lisette offers the coloring book again, asking, “May I put it on your bed?” The child accepts and begins to color.

Lisette conducts the art activity with success. She speaks to the children about the variety of emotions we all have. She says they will play a coloring game based on a game called “Basta!” (enough). She takes turns calling out emotions, and each time they must grab a crayon and color within the body outline to represent where and how much of that emotion they have until Lisette yells, “Basta!” Lisette is very lively and whips the kids up into a coloring frenzy. She begins with the emotions of fear, anger, and sadness, and ends with love and joy. I am sitting with the toddler, who is methodically drawing many tiny, blue circles on each page of her coloring book, while she listens and glances at the other children. She watches closely as a nurse enters the room and approaches the six-year-old. The boy grins and says, “It’s good that you are here. My IV is backing up.” The nurse adjusts his IV, then moves over to the toddler, preparing medicine in a syringe without a needle. The toddler opens her mouth complacently to receive it without complaint.
The fourteen-year-old has gone for a walk. I had noticed when I entered the room that she didn’t appear physically ill. She has all of her hair, and is not connected to an IV. She wore a contented, cheerful expression while she chatted on her cell phone. Soon, it is time for us to move on. The teen has returned to her bed. We all pose for photos. All the children except the toddler smile. She still appears a bit somber. I am the first to leave the room, and the teen’s caregiver follows me and grabs my arm in the hallway. She asks if I understand Spanish and begins to pour out a story to me that even with my broken Spanish, I can piece together. She is not the teen’s mother, but her aunt.
Two weeks prior, she, her two sisters and family members were traveling by car in a caravan. There was a horrible crash. The teen’s mother and father were killed. Her brother lies in critical condition in the ICU. Although the teen was unharmed, the tests she underwent at the hospital revealed that she has cancer. She had only just learned of her parents’ deaths the day before. I struggle to match that news with the image of the calm, smiling teen I’d met. Was she in shock? Denial? Is it her Faith in action?
The aunt shows me photos on her phone of her family, as well as a video about a teen whose mother dies. She says she is a Jehovah’s Witness and believes that we will all see our loved ones again after death. I tell her that I will carry her family in my heart. I think about how much good healthcare in hospitals involves helping patients and families to tell their stories. This seems true in every country I visit. And in every country thus far, families don’t hesitate to share their stories with a stranger. Perhaps it is easier to tell a stranger. But it is more than that. This woman, and others I have met, seem compelled to share their narratives, as if we couldn’t stop them if we tried.
Leaving the hospital, I am sad, exhausted and hopeful in equal measures. Lisette’s work makes a mark. Listening makes a difference. The children won’t be forgotten by us. Shared stories tear down cultural walls.

























 (photo by Jiri Kralovec)
(photo by Jiri Kralovec)
 (photo by Jiri Kralovec)
(photo by Jiri Kralovec) (photo by Jiri Kralovec)
(photo by Jiri Kralovec)
 (photo by Jiri Kralovec)
(photo by Jiri Kralovec) (photo by Jiri Kralovec)
(photo by Jiri Kralovec) (photo by Jiri Kralovec)
(photo by Jiri Kralovec) (photo by Jiri Kralovec)
(photo by Jiri Kralovec) (photo by Jiri Kralovec)
(photo by Jiri Kralovec)